
The burden of LPI on healthcare payers is staggering, with charges reaching approximately $1.5 billion annually across the US.
Introduction
Currently there are several fraudulent practices that are rampant within healthcare industry. Two critical ones among them are overcoding by providers, and human errors by claim analysts. They result in wrong payments which would then require recoupments or adjusted payments. These may lead to monetary repercussions like in case of delayed payments where Late Payment Interest (LPI) gets applied by federal mandate.
The burden of LPI on healthcare payers is staggering, with charges reaching approximately $1.5 billion annually across the US. In 2020 alone, Medicare faced nearly $200 million in LPI fees due to delayed claims processing, while private insurers reported hundreds of millions in similar costs. One in three inpatient claims submitted by providers to commercial insurers in first quarter 2023 weren’t paid for over three months and 15% of inpatient and outpatient claims were initially denied, according to data from over 1,800 hospitals and 200,000 physicians analyzed by Crowe Revenue Cycle Analytics1.
Problem Statement
My client – a large healthcare payer organization – was looking for a solution for late and erroneous claim adjudication.
To ensure accuracy of procedure codes on claims reflecting actual diagnosis and the true nature of expenses, my client employed services of a team of healthcare professionals, who reviewed each incoming claim documentation prior to approving them for adjudication. This added time to adjudicate and pay the claim. In cases when further investigation is required, the same identification may take days and may end up incurring LPI. The estimated financial impact from LPI, associated risks and requirement of new analysis teams, and loss of members due to delayed adjudication was calculated to be $6M per month.
Solutions that were considered
- Expanding the reviewing healthcare professional pool: Costly and still subject to delays.
- Paying on Good Faith: This requires reclaiming mis-adjudicated claim over-payments. While proving an immediate relief, this approach creates an imbalance in cash flow, as well as a negative user experience in cases where either providers are underpaid, or a mis-adjudication finds members ineligible for a procedure that they did not undergo and charge them for it.
My Proposed Solution
I proposed developing an ML-based application that provides confidence-based decisions through automated identification of procedure codes, depending on the claim data provided. To start, I suggested creating a Minimum Viable Product (MVP) that focuses on a single offering, limiting the ML’s identification capabilities to reviewing X-rays and determining the procedure code.
Given the client’s decades of adjudicated data with associated X-rays, I recommended leveraging this data to train a machine learning model. Hosting the model in the cloud would ensure scalability and cost-effectiveness. With the Dental claim platform processing about 150,000 claims and 40,000 X-rays per month, my proposal included having a team standardize the captured X-rays and organize the data in the proper format for training the ML model. This model would then return a procedure code along with a confidence rating.
Additionally, I proposed having another team re-engineer the claim adjudication architecture to incorporate an API call that receives the confidence-rated procedure code determination. Based on the confidence rating, the program would decide whether the procedure code should be accepted or deferred for human review.
Solution Roadmap
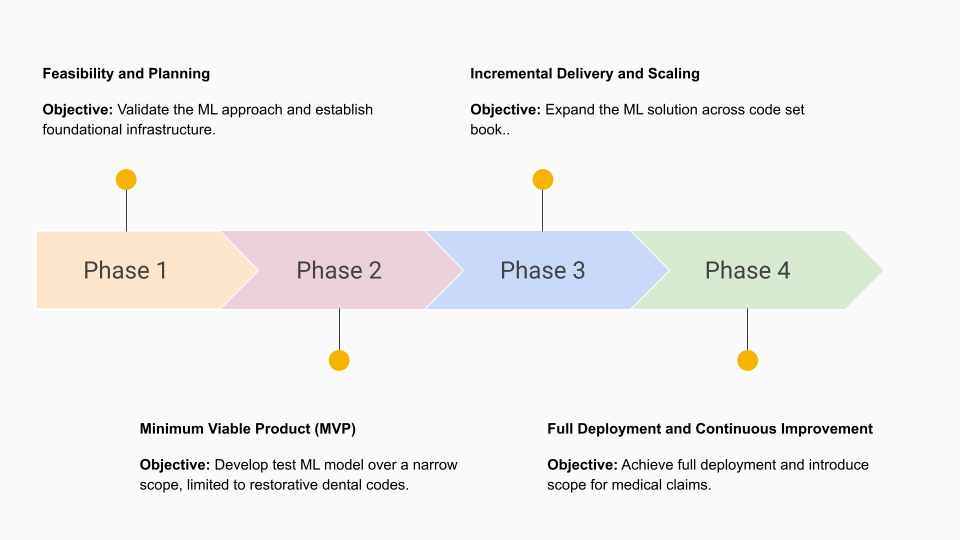
| Phase 1 | Phase 2 | Phase 3 | Phase 4 |
| Conduct feasibility study to assess the viability of ML for procedure code identification. | Data Preparation: Standardize and organize historical X-rays and procedure code data for model training. Focus on a subset of claims (Dental Restorative procedure codes) to streamline initial development. | Enhanced Model Training: Use feedback from the MVP phase to refine the ML model. Improve accuracy. Introduce scalability and availability through cloud integration. | Full Rollout: Deploy the ML solution across all claim types and fully integrate it into the claims adjudication process. |
| Define requirements and scope for the ML model. | Model Development: Build an ML model to analyse X-rays and identify procedure codes with confidence ratings. | Broader Integration: Roll out the API integration across additional procedure codes incrementally. | Ongoing Evaluation: Regularly evaluate system performance, user satisfaction, and financial impact. Continuously update the model and process based on new data and evolving needs. |
| Develop a project plan outlining timelines, resources, and key milestones. | Integration: Create API to integrate the ML model with the existing claims adjudication system. The API will receive X-ray data and return procedure codes with confidence ratings. | Monitoring and Optimization: Continuously monitor the system’s performance and accuracy. Optimize the model and integration based on real-world data and user feedback. | Innovation and Upgrades: Explore opportunities across enterprise (Medical, Behavioral, Pharmacy claims), including potential integrations with other AI technologies and expanding functionality. |
| Establish data privacy protocols to ensure compliance with PHI and PII regulations. | Testing: Pilot the MVP with a controlled set of claims (HMO claims from selected market sector alone) to validate accuracy and performance. Adjust the model based on feedback. | User Training and Support: Provide training for claim analysts and adjust workflows to accommodate the new system. Ensure support structures are in place for addressing issues and gathering user feedback. |
High Level Architecture
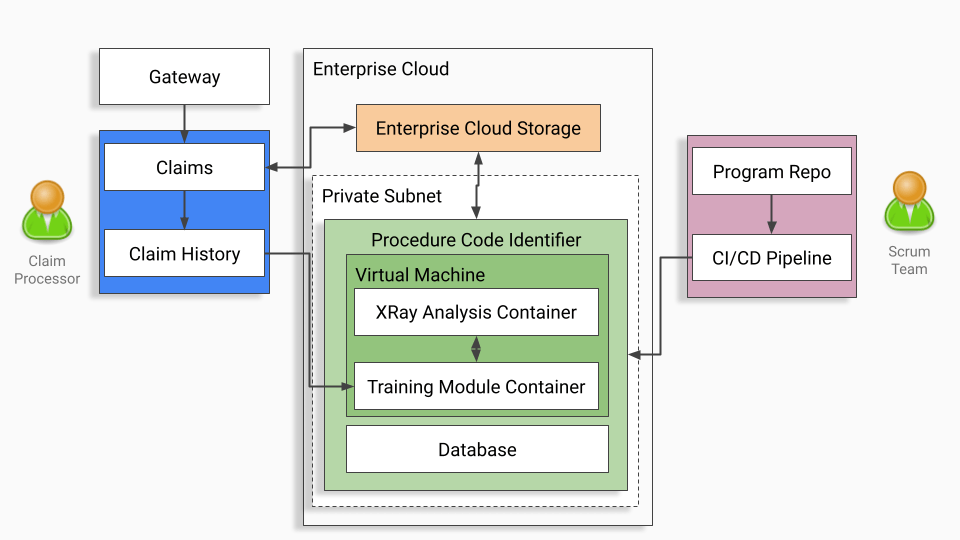
Outcome and Results
I updated my initial proposal to build an ML product in-house to leverage a Commercial Off-The-Shelf (COTS) ML product to identify procedure codes from X-Rays and related claim documentations. This reduced the adoption time. Although initially expensive to install, the cost savings from this program is set to break even before June 2025.
This project is expected to reduce procedure code determination delays from two weeks to one day, achieving an 85% reduction in processing time.
The anticipated benefits include:
- Reduced Human Intervention: Automation will cut human review needs to 5% of X-ray associated claims.
- Cost Savings: Projected savings of $720,000 per month from reduced LPI payments, and an additional $9 million annually from avoiding the need for additional team of healthcare professionals for claim reviews.
Challenges and Solutions
Data privacy concerns related to cloud infrastructure were addressed by ensuring that X-rays and claim data did not contain any Protected Health Information (PHI) or Personally Identifiable Information (PII).
Lessons Learned
This experience deepened my understanding of machine learning and neural networks. I am now more interested in pursuing opportunities to apply ML to real-world problems and drive innovation in the field.
Future Considerations
Future projects should explore various COTS products to identify the most effective solutions, considering both off-the-shelf options and homegrown developments.





Leave a comment